Streptococcal pharyngitis
Background[1]
- Peak in 5-15yr old
- Rare in <2yr of age
- Accounts for only 15-30% of pharyngitis
- Caused by S. pyogenes (Group A strep)
- Peak season is late winter / early spring
- Transmission is respiratory secretions
- Incubation period is 24-72 hours
- Antibiotics shorten symptoms by 16 hours
Clinical Features
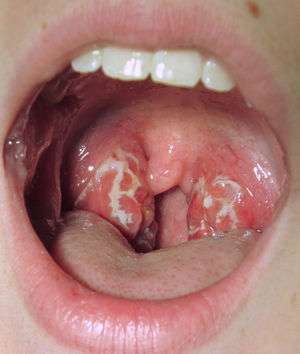
culture positive strep pharyngitis with typical tonsillar exudate
- Sore throat
- Painful swallowing
- Fever
- Nausea and vomiting
- Tonsillar exudate
- Palatal petechiae
Should NOT have a rash; if have scarlatiniform rash consider scarlet fever
Modified Centor Criteria[1]
One point is given for each of the criteria:[1]
- Absence of a cough
- Swollen and tender cervical lymph nodes
- Temperature >38.0 °C (100.4 °F)
- Tonsillar exudate or swelling
- Age less than 15^
- Subtract a point if age >44
| Points | Probability of Streptococcal pharyngitis |
|---|---|
| 1 or fewer | <10% |
| 2 | 11–17% |
| 3 | 28–35% |
| 4 or 5 | 52% |
Differential Diagnosis
- Acute rheumatic fever
- Scarlet fever
- Suppurative complications
Bacterial infections
- Streptococcal pharyngitis (Strep Throat)
- Neisseria gonorrhoeae
- Diphtheria (C. diptheriae)
- Bacterial Tracheitis
Viral infections
- Infectious mononucleosis (EBV)
- Patients with peritonsillar abscess have a 20% incidence of mononucleosis [2]
- Laryngitis
- Acute Bronchitis
- Rhinovirus
- Coronavirus
- Adenovirus
- Herpesvirus
- Influenza virus
- Coxsackie virus
- HIV (Acute Retroviral Syndrome)
Other
- Deep neck space infection
- Peritonsillar Abscess (PTA)
- Epiglottitis
- Kawasaki disease
- Penetrating injury
- Caustic ingestion
- Lemierre's syndrome
- Peritonsillar cellulitis
- Lymphoma
- Internal carotid artery aneurysm
- Oral Thrush
- Parotitis
- Post-tonsillectomy hemorrhage
- Vincent's angina
- Acute necrotizing ulcerative gingivitis
Evaluation
Rapid Antigen Detection Test Algorithm for Acute Pharyngitis[3]
| Category | Testing and Treatment |
| Clinical features strongly suggesting viral etiology (eg. cough, rhinorrhea, hoarseness, oral ulcers) |
|
| <3 years old |
|
| CENTOR = 1 |
|
| None of the above with CENTOR ≥2 |
|
Diagnostic testing or empiric treatment of asymptomatic household contacts of patients with acute streptococcal pharyngitis is not routinely recommended
Management
Antibiotics
Treatment can be delayed for up to 9 days and still prevent major sequelae
Penicillin Options:[5]
- Penicillin V 250mg PO BID x 10d (child) or 500mg BID x 10d (adolescent or adult)
- Bicillin L-A <27 kg: 0.6 million units; ≥27 kg: 1.2 million units IM x 1
Penicillin allergic (mild):[5]
- Cefuroxime 10mg/kg PO QID x 10d (child) or 250mg PO BID x 4d
Penicillin allergic (anaphylaxis):[5]
- Clindamycin 7.5mg/kg PO QID x 10d (child) or 450mg PO TID x 10d OR
- Azithromycin 12mg/kg QD (child) or 500mg on day 1; then 250mg on days 2-5
Steroids
- Consider single dose of dexamethasone 0.6mg/kg PO (Max = 10mg)[6]
Disposition
- Discharge
Complications
See Also
- Sore Throat
References
- Choby BA (March 2009). "Diagnosis and treatment of streptococcal pharyngitis". Am Fam Physician 79 (5): 383–90. PMID 19275067.
- Melio, Frantz, and Laurel Berge. “Upper Respiratory Tract Infection.” In Rosen’s Emergency Medicine., 8th ed. Vol. 1, n.d.
- Shulman, et al. Clinical Practice Guideline for the Diagnosis and Management of Group A Streptococcal Pharyngitis: 2012 Update by the Infectious Diseases Society of America. Clinical Infectious Diseases 2012;55(10):1279–82
- David Cisewski An Understated Myth? Strep Throat & Rheumatic Fever
- Shulman, et al. Clinical Practice Guideline for the Diagnosis and Management of Group A Streptococcal Pharyngitis: 2012 Update by the Infectious Diseases Society of America. Clinical Infectious Diseases 2012;55(10):1279–82
- EBQ:TOAST Trial
This article is issued from
Wikem.
The text is licensed under Creative
Commons - Attribution - Sharealike.
Additional terms may apply for the media files.