Perioral dermatitis
Background
- 90% female (increasing in males)
Etiology
- Topical or inhaled corticosteroids
- use of cosmetics,
- physical (UVB, heat, wind),
- microbiological (fusiform spirilla, candida)
- hormonal factors (premenstrual deterioration, use of oral contraceptives)
- GI tract abnormalities (malabsorption)
- emotional stress.
Clinical Features
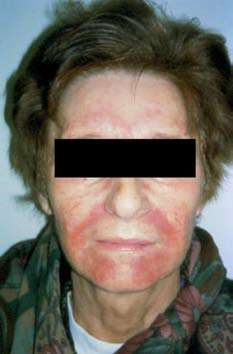
- papular, vesiculopapular and papulopustular lesions on erythematous base (Acneiform)
- confluent aspect, follicular
- location perioral, limited to skin
- typically respects rim around and 3-5 mm under lower lip, circular
Differential Diagnosis
- Rosacea
- Seborrheic dermatitis
- Acne vulgaris
- Facial demodicosis
- Lupus milliaris
- Polymorphous light reaction
- Contact dermatitis
- Haber syndrome
- Granulomatous periorificial dermatitis
Evaluation
- Usually clinical
Management
- Discontinue suspected topicals
- Rebound reaction
- hydrocortisone cuts down reaction violence
- Corticosteroid dependence - psychological follow up
- Suppression of follicular bacterial infection
- Lipophilic tetracyclines 100-250mg/d for 3-4 months
- no response - Isotretinoin
- Children - oral, topical erythromycin, metronidazole
- Antipruritics containing no corticosteroids
Complications
- Disfiguring scars - emotional
- Rebound effect, chronic course
- Lupus-like PD - dermal infiltrate, scarring
- Yellowish discoloration after diascopy
See Also
References
- Ljubojević et al. "Perioral dermatitis" Acta Dermatovenerol Croat. 2008;16(2):96-100
This article is issued from
Wikem.
The text is licensed under Creative
Commons - Attribution - Sharealike.
Additional terms may apply for the media files.